Heart Arrhythmia Treatments
in Daytona Beach, FL
Fluttering, palpitations, or a light feeling in your chest can all be potential signs you are suffering from an arrhythmia. From atrial fibrillation(afib), premature beats (PVCs), or ventricular tachycardia we can help.
No one plans on having heart problems, but if you do you need to find a doctor you can trust. At Complete Cardiology Care we staff Cardiologists and Electrophysiologists that treat patients with arrhythmias in Daytona Beach, Ormond Beach, Palm Coast, Deltona, Deland, and the surrounding areas.
4 Million
Suffer from recurrent
arrhythmias in the U.S.
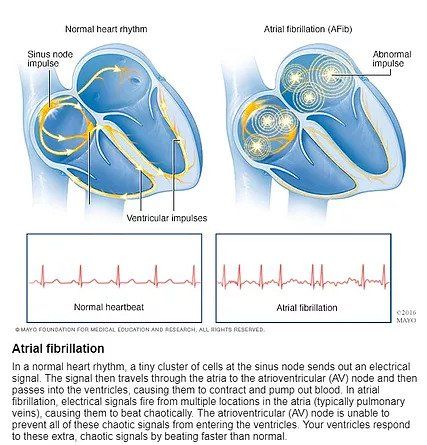
Atrial fibrillation
Most common arrhythmia diagnosed
65-70
Mean age of Afib diagnosis.
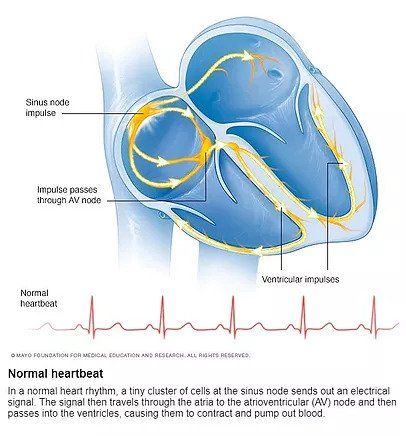
A Normal Heart Beat
What is a heart arrythmia?
Heart rhythm problems (heart arrhythmias) occur when the electrical impulses that coordinate your heartbeats don't work properly, causing your heart to beat too fast, too slow or irregularly.
Heart arrhythmias may feel like a fluttering or racing heart and may be harmless. However, some heart arrhythmias may cause bothersome — sometimes even life-threatening — signs and symptoms.
Heart arrhythmia treatment can often control or eliminate fast, slow or irregular heartbeats. In addition, because troublesome heart arrhythmias are often made worse — or are even caused — by a weak or damaged heart, you may be able to reduce your arrhythmia risk by adopting a heart-healthy lifestyle.
Don't let your arrhythmia control your life and get treated today
If you are curious how we can help you with your arrhythmia symptoms, please reach out to us. We are currently accepting new patients. Complete Cardiology Care staffs Cardiologists and Electrophysiologist that serve patients in Ormond Beach, Daytona Beach, New Smyrna Beach, Port Orange, Deltona, Deland, and the surround areas.
Our Cardiologists and Electrophysiologists take nearly all insurances. We accept Aetna, AARP Medicare Complete, Blue Cross / Blue Shield, Cigna, Florida Healthcare, Florida Hospital Care Advantage, Freedom Health, Health First Health, Humana PPO - out of network benefits apply, Medicare, Optimum Healthcare, Railroad Medicare, Tricare, United Healthcare, VHN, Wellcare.
We are also a partner with the VA and are proud to serve those who have served our country!
Self Pay Cardiology services are available too! Call and ask for our price list.

